Skip Maine state header navigation
Health Status and Needs Assessment
of Native Americans in Maine:
Final Report
Paul Kuehnert, M.S., R.N.
Director, Division of Disease Control
Maine Bureau of Health
January 15, 2000

Maine Department of Human Services
Bureau of Health
11 State House Station
Augusta, Maine 04333-0011
Angus S. King, Jr. Governor Kevin Concannon, Commissioner Dora Anne Mills, MD, MPH Bureau Director
In accordance with Federal laws, the Maine Department of Human Services does not discriminate on the basis of sex, age, color, or national origin or disability in admission or access to, or treatment or employment in its programs and activities. The Department Affirmative Action Coordinator has been designated to coordinate our efforts to comply with and implement these federal laws and can be contacted for further information at 221 State Street, Augusta, Maine 04333 (207)287-3488 (voice), or Maine relay 711 (TTY).
Acknowledgements
This report would not have been possible without the cooperation, information, and insights provided by the directors and staffs of the Native American health centers in Maine. The health directors are:
- Brian Altvater, Passamaquoddy tribe—Pleasant Point, Maine
- George Bear, Penobscot Nation – Indian Island, Maine
- Elizabeth Martin, Passamaquoddy tribe – Indian Township, Maine
- John Oulette, Aroostook band of Micmac Indians --- Presque Isle, Maine
- Michelle Tarr, Houlton band of Maliseet Indians, Houlton, Maine
Additionally, a number of staff from the Maine Department of Human Services’ Bureau of Health and Bureau of Medical Service made key contributions to this report. They include: Cathy St. Pierre and Brenda Corkum of the Office of Data, Research and Vital Statistics; Michael Day of the Bureau of Medical Services; Nancy Sonnenfeld, Patricia Jones, Barbara Leonard, Fredricka Wolman and Judith Graber of the Division of Family and Community Health; Dorean Maines, Office of Health Data and Program Management; Mark Griswold, Michelle Mosher, Linda Huff, Sally Lou Patterson, Robert Burman, and Marlene Crosby of the Division of Disease Control; Andrew Smith, State Toxicologist; and Dora Anne Mills, Director of the Bureau of Health.
Background
In the late summer of 1999, Mr. Irvin Rich of the U.S. Health Care Financing Administration (HCFA) requested that Maine Bureau of Health (BOH) participate in a conference that was being planned for October. The conference, jointly sponsored by HCFA and the U.S. Health Resources and Services Administration (HRSA) and the Indian Health Services (IHS), was being organized to address the feasibility of developing collaborative efforts to address health disparities experienced by Native Americans in New England. The conference was to be attended by representatives of New England states’ health and Medicaid programs, private and public universities and colleges, and health and political leaders from the region’s Native American tribes. The Maine BOH was asked to prepare an assessment of the health needs of its Native American residents for presentation to the conference. A preliminary, verbal presentation of the assessment findings was made to the conference participants meeting in Boston, Massachusetts on October 5, 1999. This final, written report is based upon that presentation.
Goals and Methods
The goals of this health needs assessment and analysis of the Native American population of Maine were:
- To provide an overview of the population’s health status;
- To identify priority health needs;
- To identify health resources and assets;
- To identify health service/resource gaps, and
- To identify possible areas for action to improve the health of Native American residents of Maine that could be taken by the Maine Bureau of Health.
The assessment and analysis were guided by the epidemiological approach to community needs assessment (Finnegan and Ervin, 1989). Specific methods included:
- Review of population data on socio-economic status, natality, morbidity and mortality data. All data were compared to the rest of the Maine population for reference purposes. (Natality and mortality data were gathered for the twenty year period 1978-1997 and grouped in five year increments (see discussion in Limitations below.))
- Review of a recent report on a behavioral risk factors survey of one specific Maine Native American sub-population.
- Interviews with key informants.
Limitations
A number of important potential limitations related to the interpretation of the findings of this assessment and analysis must be noted at the outset. First and foremost, the Native American population in Maine is relatively small (approximately 6,500 individuals per the 1990 census). As a result, the number of health-related events (births, illnesses, deaths) are relatively few each year and are unstable from a statistical standpoint. In order to address this problem, natality and mortality data were grouped into five year time periods to enhance their stability and improve the ability to interpret trends. Even so, the reader should note that all underlying numbers are small and must be interpreted with caution.
A further complication related to the already-small numbers of health related events amongst the Native American population in Maine is the strong possibility that some data elements from the vital records may not be reliable due to reporting error. A number of studies (Hahn and Eberhardt, 1995) have documented that in a significant number of death certificates in the U.S., race/ethnicity is improperly recorded. Two separate studies ( Hahn and Eberhardt, 1995 and Sorlie et al, 1992), found a misclassification ratio of roughly 0.82 of race on the death certificates of Native Americans. When using mortality data as one measure of health problems in a population, this error has the effect of underestimating the impact of a disease or health problem on the population in which the deaths are misclassified. The implications for this needs assessment are discussed in the Recommendations section of this report.
Two additional potential limitations regarding this needs assessment are: 1) the limited time and resources available for the assessment, and 2) the historical role of the Bureau of Health in relation to Native American health in Maine. As to the first issue, while every effort was made to be thorough and comprehensive, the lack of resources did have the effect of limiting the type and extent of data gathering and analysis activities. For example, key informant interviews were limited to tribal health leaders and their key staff. Additional time and resources would have allowed us to interview and/or survey additional community leaders and members.
Regarding the second issue, the Maine Bureau of Health has played a relatively minor role in addressing the health of Native Americans in Maine. This has been due to primarily two reasons: 1) the central role of direct federal involvement with Maine’s tribes historically through the Indian Health Service (IHS) and 2) the evolution of tribal autonomy and self-governance in relation to social and health services over the past twenty-five to thirty years. Thus, the Bureau of Health does not have well-established, longstanding relationships with Maine’s tribal health leaders. This, as a result, may have inadvertently limited the information shared in key informant interviews, as well as limiting the depth of the analysis of the information that was shared.
Overview of Native Americans in Maine
Maine, the largest state in New England, has approximately 1.2 million residents. Taken as a whole, Maine’s residents are relatively poor, as compared to national and regional averages, and live primarily in rural settings. The vast majority (98.5%) of Mainers are white, with the largest racial minority groups in the population being Asian-Pacific Islanders (0.7%) and Hispanics (0.7%), followed by Native Americans (0.5%) and African-Americans (0.5%) (percentages add to greater than 100% due to individuals with multi-racial heritage.)
While Maine’s Native Americans live in every county in Maine and each of its cities, the vast majority resides in or near the five small, rural communities of Indian Island (Penobscott Nation), Pleasant Point (Pasamaquoddy tribe), Indian Township (Pasamaquoddy tribe), Houlton (Houlton Band of Maliseet) and Presque Isle (Aroostook Band of Micmac) illustrated in Figure 1. With the exception of Presque Isle, each of these communities includes a reservation where many tribal members live. The Micmacs have only been federally recognized relatively recently and do not have a reservation. Micmacs live throughout Aroostook County and have tribal government offices, a community center, health center and some housing developments in Presque Isle.
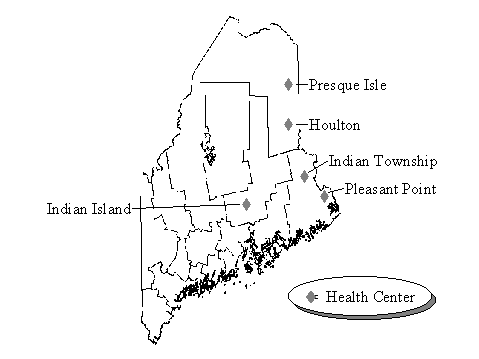
Figure 1
Tribal governments in Maine, as in other parts of the U.S., have unique, direct and fairly complex relationships with the federal government as well as with the State. For the purposes of this assessment, it is important to note that tribal members have all the rights and responsibilities of other Maine citizens, including access to health and social services. Most often, these services – e.g., social services for children or elders -- are delivered under contract with the tribal government as opposed to being delivered by townships or state employees. This is also true for housing and environmental protection programs as well.
Each of Maine’s tribes receives funding directly from the IHS. The level of funding is set according to an IHS allocation formula based on the number of tribal members. These funds allow each tribe to operate its own community health center and community health programs. These range from the comprehensive primary care health centers that have been operated by the Penobscott and Pasamaquoddy tribes for nearly thirty years, to the recently established centers of the Maliseet and the Micmac bands which provide limited direct services while purchasing a more extensive set of services from other community providers. However, IHS funds derived from this same allocation formula must also be used to purchase diagnostic, treatment and rehabilitation services for un- or under-insured tribal members. This, in turn, makes funding for preventive and primary care services for each tribe vulnerable to unanticipated, often catastrophic events (e.g., car wrecks with serious injuries) befalling individual members. (These issues are more fully discussed in the Health Resources and Conclusions sections of this report).
Population Comparisons
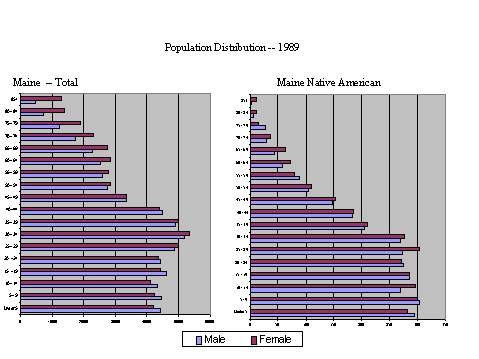
The Native American population in Maine is younger than the general population. The population distributions are displayed in Figure 2. The population distribution of Maine Native Americans is similar to distributions of developing nations.
Figure 2
As detailed in Table 1, Maine Native Americans have lower per capita and household incomes than those of Mainers as a whole ($7,840 and $21,519 versus $12,957 and $27,854 respectively), higher rates of unemployment (14.4% versus 6.6%), and lower rates of attaining a high school education or higher (69% versus 78.8%).
|
Table I POPULATION COMPARISONS |
||
|
MAINE |
MAINE NATIVE AMERICANS |
|
|
POPULATION |
1,227,928 |
6,392 |
|
EDUCATION High School or higher BA or higher |
78.8% 18.8% |
69.0% 7.7% |
|
INCOME Per capita Median Household Median Family |
$12,957 $27,854 $32,422 |
$7,840 $21,519 $23,493 |
|
EMPLOYMENT In labor force Unemployed |
65.6% 6.6% |
64.5% 14.4% |
Natality Comparisons
As detailed in Table II, the birth rate of Maine Native Americans has been higher than that of the entire population of Maine during the 1978-1997 period. This is consistent with the population distribution noted above (Figure 2). The percentage of births that are low birth weight (<2500 grams) among Maine Native Americans has averaged 5.3% with little variation during the past twenty years and is the same as the average of the Maine population as a whole (Table II).
|
Table II NATALITY COMPARISONS |
||
|
MAINE |
MAINE NATIVE AMERICANS |
|
|
LIVE BIRTHS PER 1,000 POPULATION: 1978-1982 1983-1987 1988-1992 1993-1997 |
14.5 14.2 13.8 11.4 |
21.0 16.2 15.1 16.4 |
|
BIRTHS < 2500 grams % OF ALL BIRTHS 1978-1982 1983-1987 1988-1992 1993-1997 |
5.2% 5.3% 5.1% 5.8% |
5.6% 5.8% 4.5% 5.3% |
Births to Maine Native American teenagers have been consistently higher ---ranging one and one-half to two times higher --- than births to all Maine teenagers (Table III.) The Maine Native American Teen birth rate apparently declined dramatically between the first and second five year period (from 94.7 to 63.6 births per thousand teen women), but then has remained apparently stable. The average and median ages of Maine Native American teen mothers (17.6 and 18 years respectively) has remained virtually unchanged during the twenty year period and is about the same as that of all Maine teen mothers (17.9 and 18 years respectively).
|
Table III Teen Birth Comparison |
||
|
ALL MAINE TEENS |
NATIVE AMERICAN TEENS |
|
|
Birth rate/1000 Females 15 – 19 years old: 1978-1982 1983-1987 1988-1992 1993-1997 |
45.6 40.4 41.3 34.1 |
94.7 63.6 68.7 67.1 |
As illustrated in Table IV, infant deaths amongst both Maine Native Americans and Mainers as a whole reached record low rates of 6.4 and 5.7 deaths per 1000 live births respectively during the last five year period. Maine as a whole has shown a slow and steady decline in infant deaths over the twenty year period. Maine Native Americans began and ended the period with rates comparable to that of the general population, but there were wide, upward fluctuations in the middle ten years, especially in the 1988-92 period. These fluctuations must be viewed with considerable caution, however, since the underlying numbers are extremely small.
|
Table IV Infant Mortality Comparison |
||
|
ALL MAINE |
MAINE NATIVE AMERICANS |
|
|
Infant deaths/1000 live births: 1978-1982 1983-1987 1988-1992 1993-1997 |
9.7 8.5 6.6 5.7 |
9.4 10.1 20.3 6.4 |
Mortality Comparisons
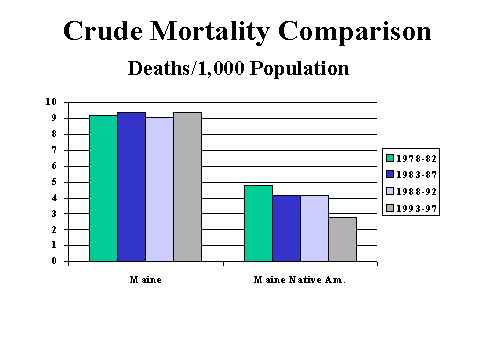
Also consistent with having a younger population, crude death rates among Maine Native Americans over the twenty year period are much less than those of the general population (average of 4.0 versus 9.3 deaths per thousand, see Figure 3).
Figure 3
However, life expectancy among Maine Native Americans is less than that of all Mainers. Mean and median ages of death are compared between the two for each five year period in Table V. While exercising caution in interpretation given the small numbers involved for Maine Native Americans, it appears that gains are being made (increasing average age of death from 55 to 60 years) but that the gap between the two populations has not apparently narrowed.
|
Table V Age at Death Comparison |
||
|
ALL MAINE |
MAINE NATIVE AMERICANS |
|
|
Mean and Median Age of all Decedents, all causes: 1978-1982 1983-1987 1988-1992 1993-1997 |
Mean Median
74.1 77.0 |
Mean Median
60.1 63.0 |
Crude numbers of deaths to Maine Native Americans by Cause Grouping are detailed in Table VI. Leading causes of death for Maine Native Americans have been converted into age adjusted rates and compared to age adjusted rates for the Maine general population in Table VII.
|
Table VI Deaths to Maine Native Americans by 32-cause grouping 1978-1997 |
||||
Cause |
1978-1982 |
1983-1987 |
1988-1992 |
1993-1997 |
|
INFECTIOUS & PARASITIC DISEASES(001-139) |
2 |
3 |
1 |
2 |
|
MALIGNANT NEOPLASMS (140-208) |
14 |
19 |
31 |
27 |
|
DIABETES MELLITUS (250) |
|
1 |
4 |
4 |
|
NUTRITIONAL DEFICIENCIES (260-269) |
|
|
2 |
|
|
ANEMIAS (280-285) |
|
1 |
|
|
|
MENINGITIS (320-322) |
|
1 |
|
|
|
HEART DISEASE (390-398,402,404-429) |
33 |
22 |
21 |
16 |
|
CEREBROVASCULAR DISEASE (430-438) |
12 |
5 |
4 |
2 |
|
ATHEROSCLEROSIS (440) |
|
1 |
1 |
|
|
OTHER DIS ARTERIES & CAPIL (441-448) |
1 |
1 |
3 |
1 |
|
PNEUMONIA AND INFLUENZA (480-487) |
4 |
4 |
2 |
1 |
|
CHRONIC OBSTR PULMONARY DIS (490-496) |
2 |
5 |
9 |
5 |
|
ULCER OF STOMACH & DUODENUM (531-533) |
|
1 |
|
|
|
ABDOM HERNIA & INTEST OBS (550-553,560) |
|
1 |
|
|
|
CHRONIC LIVER DIS & CIRRHOSIS (571) |
3 |
5 |
1 |
1 |
|
NEPHRITIS,NEPH SYND & NEPHROSIS(580-589) |
|
1 |
1 |
1 |
|
CONGENITAL ANOMALIES (740-759) |
|
2 |
3 |
|
|
PERINATAL CONDITIONS (760-779) |
|
2 |
2 |
1 |
|
SYMPTOMS, SIGNS & ILL-DEF COND (780-799) |
3 |
1 |
3 |
1 |
|
ALL OTHER DISEASES (RESIDUAL) |
7 |
8 |
19 |
9 |
|
ACCIDENTS & ADV EFF (E800-E949) |
11 |
13 |
11 |
4 |
|
SUICIDE (E950-E959) |
2 |
4 |
2 |
4 |
|
HOMICIDE & LEGAL INTERV (E960-E978) |
3 |
1 |
3 |
|
|
ALL OTHER EXTERNAL CAUSES (E980-E999) |
|
|
1 |
|
|
ALL CAUSES |
97 |
102 |
124 |
79 |
|
Table VII Mortality Comparisons Age-Adjusted Deaths by Cause, Per 100,000 Population |
||||||||
|
|
1978-1982 |
1983-1987 |
1988-1992 |
1993-1997 |
||||
|
|
All
|
Native
|
All
|
Native
|
All
|
Native
|
All
|
Native
|
|
Breast Cancer |
23.0 |
27.4 |
22.0 |
7.7 |
22.1 |
25.0 |
20.2 |
16.7 |
|
Lung Cancer |
37.7 |
40.7 |
39.6 |
50.0 |
43.4 |
56.0 |
43.5 |
61.7 |
|
Cardio-vascular Disease |
244.1 |
357.8 |
220.8 1 |
80.1 |
178.9 |
143.1 |
160.0 |
80.5 |
|
Heart Disease |
193.0 |
254.2 |
179.3 |
135.7 |
143.3 |
103.4 |
127.4 |
69.6 |
|
Cerebro-vascular Disease |
36.1 |
95.4 |
28.1 |
32.3 |
23.9 |
20.3 |
22.9 |
7.6 |
|
Suicide |
12.9 |
10.3 |
12.6 |
14.3 |
12.3 |
7.9 |
11.7 |
15.1 |
|
Motor Vehicle Crashes |
20.3 |
34.5 |
17.9 |
23.2 |
16.7 |
15.1 |
14.3 |
6.4 |
|
Diabetes |
8.6 |
0.0 |
9.0 |
6.4 |
12.8 |
21.6 |
12.8 |
16.9 |
|
Any Mention Diabetes |
36.9 |
39.3 |
41.0 |
63.4 |
39.9 |
80.5 |
40.3 |
36.6 |
Over the past twenty years, the leading cause of death among Maine Native Americans has shifted from cardiovascular diseases (ICD9 390-398, 402, 404-438) to cancer (ICD9 140-208). In the 1978-82 period, cardiovascular disease accounted for 46% of deaths in Maine Native Americans while cancer accounted for 14.4%. In the 1993-97 period, cardiovascular-related deaths dropped to 22.7% while cancer increased to 34%. This is in contrast with the general population of Maine in which heart disease remains the leading cause of death (30%) while cancer is the second leading cause (25%) (Maine Department of Human Services, 1999, page III 13).
As shown in Figure 4, the rate of deaths due to lung cancer among Maine’s general population appears to have increased slightly over the past twenty years. During the same time period, comparable rates among Maine Native Americans appear to have increased more dramatically. Lung cancer accounted for 42% of all cancer deaths to Maine Native Americans (Figure 5) during this twenty year period.
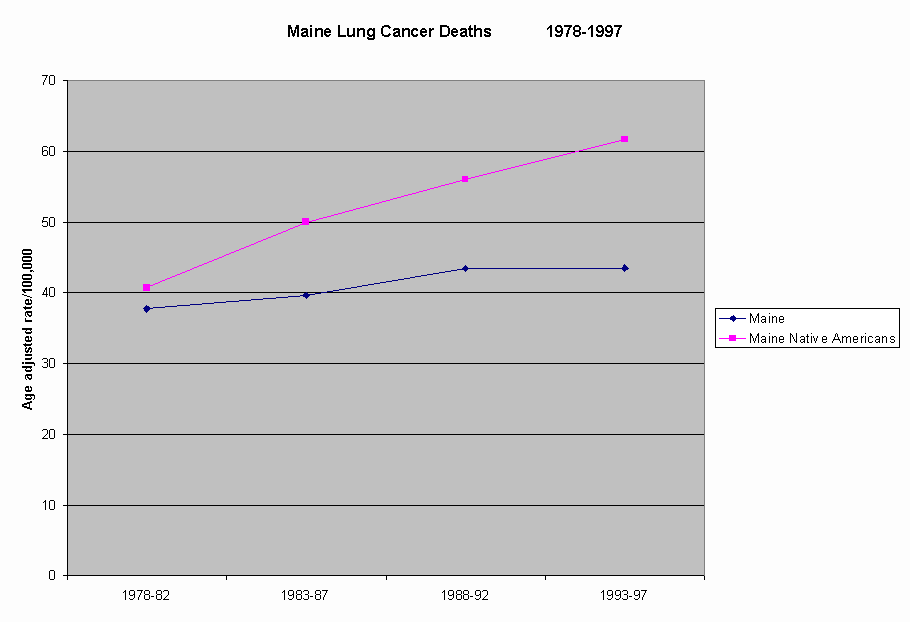
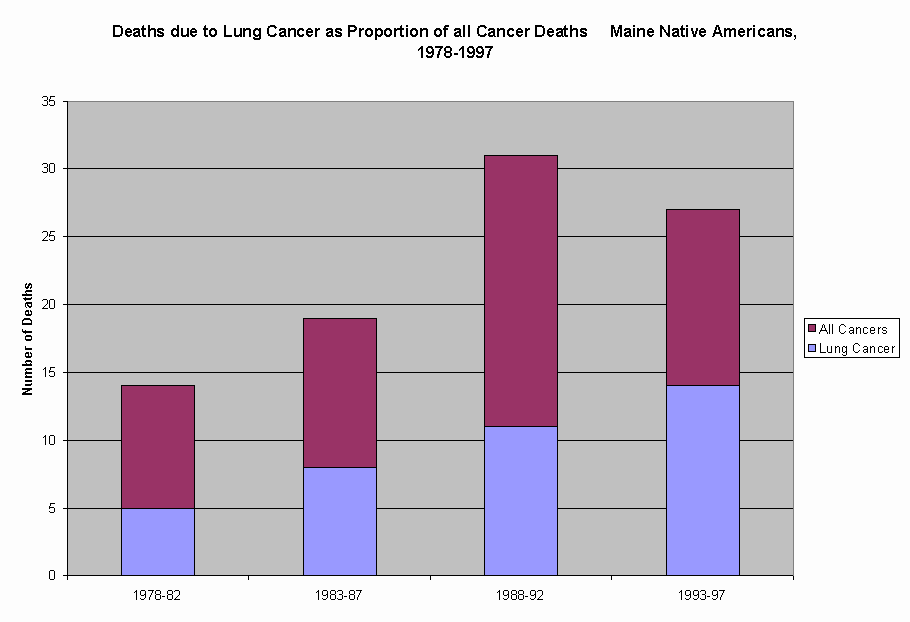 Figure 4
Figure 4
Figure 5
The apparent excess burden of deaths due to lung cancer in Maine Native Americans may reflect increased rates of tobacco use (see Morbidity and Other Health Concerns section below).
On the other hand, the rate of deaths due to cardiovascular disease among Maine Native Americans compare extremely favorably with the same rate in the general population in Maine (Figure 6). The apparent dramatic declines in death rates related to cardiovascular disease are reflected in specific components of the Cardiovascular disease cause grouping, including both Heart Disease (Figure 7) and Cerebrovascular Disease (Figure 8).
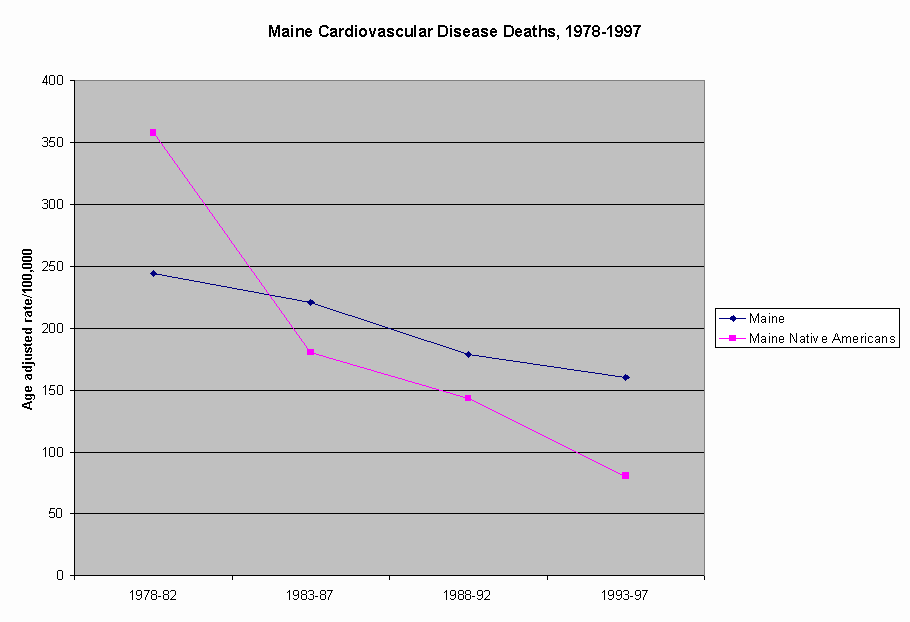
Figure 6
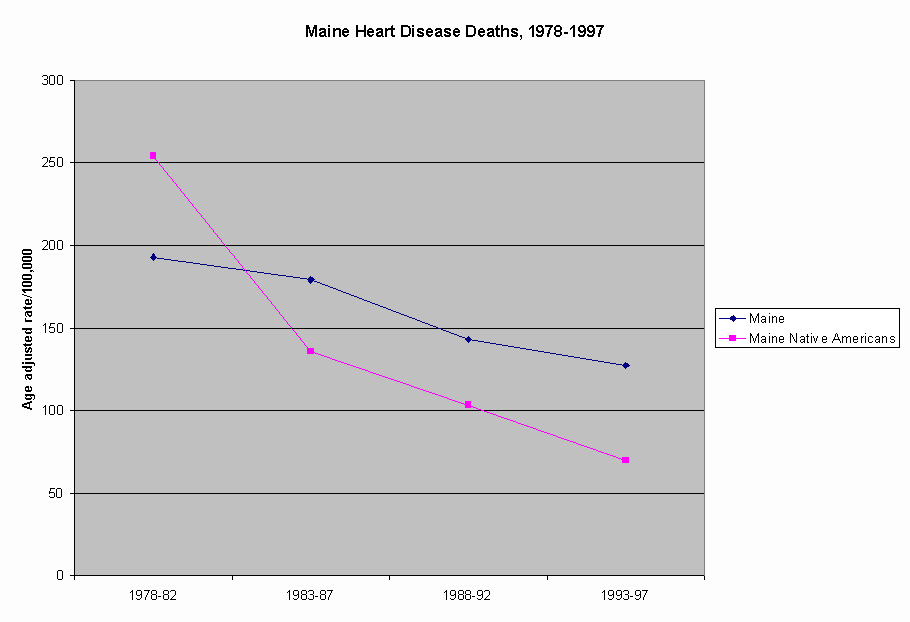 Figure 7
Figure 7
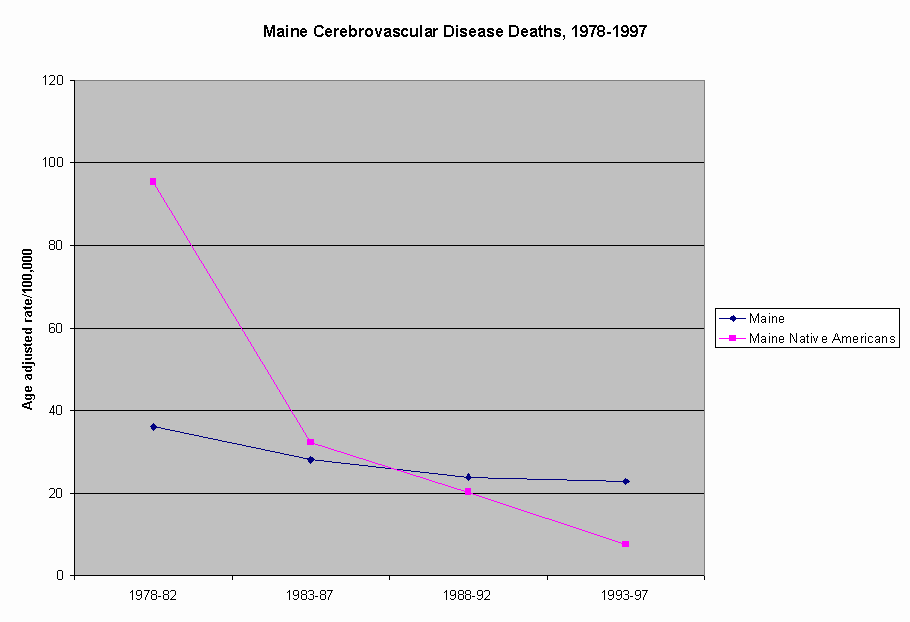
The apparently significant decline in rate of deaths due to cardiovascular disease in Maine Native Americans and their dramatic difference with the comparable rates in Maine’s general population requires in-depth evaluation. Preliminarily, it seems that at least three factors may play a role: changes in the population denominator, misclassification of race on death certificates and increasing access to preventive health information and services.
First, some part of the decline may be explained by the dramatic increase in Native American population in Maine, from just over 4,000 reported in the 1980 census to over 6,300 in the 1990 census. This increase suggests changes either in the accuracy of census methods and/or the increase in Mainers of mixed racial heritage in identifying themselves as Native Americans. Secondly, it has been documented that death certificates are often inaccurate in recording the race of the decedent (Hahn and Eberhardt, 1995). As noted above, such a misclassification would have the effect of understating the impact of cardiovascular disease on Maine Native Americans. Thirdly, medical primary care was made easily accessible and combined with community-based, culturally relevant primary and secondary prevention services were created by and implemented in each of the reservation communities in Maine by the tribal health centers during this time period. People at high risk of cardiovascular disease were targeted for these programs and services. It is important that the contribution of each of these factors to the overall decrease in the rate of deaths from cardiovascular disease in Maine Native Americans be determined. (See Recommendations section)
In all other respects, mortality among Maine Native Americans is very similar to all Mainers. Those areas with apparent differences (See Table VII above) ---e.g., suicide, motor vehicle crashes, and diabetes--- have underlying numbers that are so small and unstable that little can be inferred from either the differences between the two populations or the variance in the Maine Native American rates from period to period.
Morbidity and Other Health Concerns
Current, key health problems facing Maine’s Native American were elicited from the tribal health directors and their staffs during the interviews. Consistently, the top three problems facing the population were identified as being:
- Diabetes and its complications
- Addictions: tobacco, alcohol, other substances
- Obesity
These perceptions of the key informants were verified by examining two data sources. First, Medicaid claims data for 1997 from the Maine Bureau of Medical Services were analyzed to determine the most frequent diagnostic categories for health problems diagnosed during outpatient visits to the five health centers. These data, summarized in Table VIII, while not necessarily representative of the Maine Native American population as a whole, provide a snapshot of morbidity for what could be argued may be the most vulnerable portion of that population. The frequency of outpatient diagnoses related to diabetes, mental illness and chemical addiction, respiratory diseases, and cardiovascular diseases can be said to confirm the key informants reports.
|
Table VIII Top Seven Morbidity Categories Medicaid Claims from Maine Native Americans, 1997 |
|
The second data source reviewed was the recent Behavioral Risk Factor Survey conducted by the Aroostook band of Micmac Indians in 1998. This survey was reviewed for this assessment because it was the most recent conducted among any Native American population in Maine. Key findings regarding self reported health behaviors are summarized in Table IX. These findings of higher tobacco use, higher percentage of overweight and leading sedentary lifestyle, and higher percentage of problem alcohol use are consistent with the problems identified by the key informants.
|
Table IX Summary of Key Findings: Behavioral Risk Factor Survey Aroostook Band of Micmac Indians, 1998 |
|
Finally, although not clearly linked to disproportionate Native American morbidity at present, many of the key informants expressed deep concern about two other health issues: environmental toxins and HIV/AIDS. Environmental concerns were focused on mercury, dioxin, lead, and cadmium. A number of studies regarding these toxins are underway. Besides concerns regarding near-term impact of these toxins on individual health, more long term concerns were voiced regarding the potential negative spiritual and community health impact should traditional reliance on hunting and fishing be restricted due to environmental pollution.
HIV/AIDS has had a relatively small impact on Native American communities in Maine to date. The key informants did express concern about its potential for having a devastating impact on their communities in the future. In two of the five tribal areas, a particularly high degree of concern was voiced regarding the growing prevalence of injection drug use among some tribal members and its potential as a pathway for HIV’s entry into the community.
Health Resources
Each of Maine’s tribes owns and operates its own health center. These centers were established with IHS and tribal funding. The centers range from the comprehensive primary care health centers that have been operated by the Penobscott and Pasamaquoddy tribes for nearly thirty years, to the more recently established (less than 5 years old) centers of the Maliseet and the Micmacs bands. The scope of services delivered on-site at the health centers varies. In every case, though, a full array of primary care services are offered to tribal members either on site or by local providers in nearby communities. These include: medical primary care, dental care, basic laboratory and x-ray services, pharmacy services, home health, and outpatient mental health and chemical addiction treatment services.
Besides directing the operations of the health centers, the tribal health directors also oversee the provision of some local public health services. These include a variety of primary prevention and wellness programs directed toward both their tribal members as a community and at-risk groups within the tribal communities. The health directors also either direct or collaborate with other leaders in their tribal governments the provision of environmental health services (e.g., lead, dioxin, etc.) and public sanitation (e.g., drinking water, food services, etc.).
Finally, each tribal health director oversees the purchase of needed physical and mental health diagnostic, in-patient treatment and rehabilitation services for un- or under-insured tribal members. Essentially, each tribe is the "health insurer of last resort" for all of its members. An assigned health center staff member(s) provides case management services for tribal members, coordinating coverage with other insurers and negotiating payment for services for members with no other health insurance.
These health resources are limited by two key factors: funding and availability of health professionals and facilities. In regards to funding, all of these health services --- local public health, primary care services, and secondary/tertiary care purchasing --- come out of each tribe’s or band’s health budget. Revenues are provided largely by a formula-based allocation from the IHS. According to the tribal health directors, this allocation is and has been essentially flat. This base funding may be supplemented by the tribes and/or by competition for categorical grants obtained from outside sources, such as the Bureau of Health or the Department of Environmental Protection. This funding approach has the effect of making funds for preventive and primary care services for each tribe vulnerable to unanticipated, often catastrophic events (e.g., car wrecks with serious injuries) befalling individual members.
Beyond these tribal health resources, availability of health professionals and facilities is limited for Native Americans in Maine. This is true for most other Maine residents as well. As shown in Tables X and XI below, these shortages are even more acute in the very rural, remote areas of the state (Aroostook and Washington counties) in which the reservations are located.
|
Table X Health Resources: Professionals |
||||
|
Maine |
Aroostook County |
Penobscot County |
Washington County |
|
|
Physicians Primary Care Physician* Phys. Asst.* R.N.* Dentist* Dental Hygen* Drug Counslr* Counselor* *per 100,000 population |
1:512
85 25 1,183 48 75 59 87 |
1:749
60 26 1,072 33 46 31 14 |
1:478
80 37 1,350 44 79 68 98 |
1:861
71 8 784 30 41 44 44
|
|
Table XI Health Resources: Facilities |
||||
|
Maine |
Aroostook County |
Penobscot County |
Washington County |
|
|
Hospital Beds* Long Term Care Beds** Res. Care Level I Beds* Res. Care Level II Beds* *per 1,000 population **per 1,000 population > age 65 |
3
57
1.4
3.5 |
3.5
60
1.8
4 |
4
50
1.8
2 |
2.4
55
1.8
2.5 |
These shortages are further exacerbated by the need for culturally competent providers, i.e., providers who are familiar with, sensitive to, and respectful of Native American culture.
Barriers to Health
The tribal health directors and their staff members were asked to identify barriers to health experienced by their members. Each of the following barriers were identified as key by directors and/or staff at three or more of the five tribal health centers:
- Transportation:
public transportation is non-existent in these very rural, remote communities. Distances that must be traveled range from a few miles to clinic-based services to hundreds of miles for many diagnostic procedures and specialty care. In most cases, individuals must provide their own or rely on family and friends for transportation to and from both clinic and remote services.- Low income:
tribal members’ low income has multiple effects on health, including: poor nutrition, inability to maintain personal vehicles for transportation, and multiple economic concerns/stressors that may have higher priority than health concerns.- Prejudice and racism:
The tribes and tribal members continue to experience racially based discriminatory practices and attitudes in the broader community. These attitudes and practices are both barriers to health care and negative stressors affecting individual and community health.- Shortages of qualified personnel:
All of the Indian health centers in Maine are located in designated health manpower shortage areas (See discussion above in the Health Resources section of this report) . Shortages of mental health and substance abuse treatment professionals are most acute at present.- Inadequate funding:
As discussed in the Health Resources section of this report, IHS funding for the Maine tribes is flat and must provide both individual member insurance coverage as well as support for primary and secondary prevention programs. The demand for health services and need for population-level prevention and wellness programming continues to grow, risking significant and growing gaps in services for tribal members.- Inaccessible/culturally inappropriate mental health and chemical addiction in-
and day-treatment facilities. In addition to shortages (noted above and in the Health Resources section of this report) of qualified, culturally competent mental health and substance abuse treatment professionals to staff outpatient services at the Indian health centers, there are no culturally competent in-patient or day-treatment facilities and programs in all of northern Maine. As a result, community members must be hospitalized a minimum of roughly 200 miles away (Portland, Me) or even further for treatment. For example, young Native Americans must be placed out of state (North Carolina) if they need a Native American culturally based treatment program.- Environmental toxins
including dioxin, mercury, lead, arsenic and cadmium are perceived as major threats to the health of Maine Native Americans. These perceived threats act as barriers to tribal members following traditional lifestyles and have a negative impact on health and well being.
Strategies to improve the health of Maine’s Native American population must address these barriers if the strategies are to succeed.
Community Assets
The tribal health directors and their staff members were asked to identify community assets that could be mobilized to address health concerns or problems faced by their tribes. Each of the following assets were identified as key by directors and/or staff at three or more of the five tribal health centers:
- Talented and committed health leadership and staff
have been recruited and retained by each of Maine’s tribes. Many of the tribal health directors and a number of key staff have been in their positions for more than a decade, providing continuity to their relatively young organizations.- Community norms and values
that are based on traditional Native American culture strongly emphasize family ties, the importance of children, and compassion and caring for the community.- Community attitudes
that are supportive of and concerned about the health and well being of the individual, family and community. This is reflected in active commitment by tribal political leaders to the health centers and health programs.- The tribes and tribal leaders are politically experienced and knowledgeable. A successful track record on a variety of issues on the state and federal levels has been established over the past twenty-plus years.
- Health centers and health funding are in place.
Although levels of support are not as high as needed, the existing resources are tremendous community assets for health.
Conclusions
This brief assessment of Native Americans in Maine has provided an overview of the health status and health needs of our state’s second largest minority community. Significant improvements in the health status of the Native American population appear to have been made over the past two decades. These improvements are the direct result of a comprehensive effort, funded largely by the federal Indian Health Services and directed by leadership from each tribe, to provide comprehensive primary health care services to Maine’s Native Americans. Health disparities between the Native American and the general, majority white population of Maine, while not resolved, are being successfully addressed.
But much remains to be done. Attention to increasing the health resources available to the tribes is vital at this time or the gains that have been made will be lost. Key to building on the success of Maine’s tribes in addressing the question of access to primary care will be sustaining and enhancing access to primary and secondary care, particularly around the key problem areas of chemical addiction and mental illness. Just as important will be to further develop and then maintain population-focused, primary prevention efforts that will succeed in reducing the incidence of chronic disease, particularly those related to smoking, inactivity, substance use, and poor nutrition. Finally, of particular importance will be strategies to secure these resources while separating it from funding for individual tribal member major medical coverage, especially catastrophic coverage.
Recommendations
The Maine Bureau of Health should take steps to formalize working partnerships with Maine’s five tribal health centers. A short-term agenda that could be addressed through such partnership efforts would include two key objectives:
- Completing an in-depth evaluation
of the apparent dramatic reduction in mortality from cardiovascular disease among Native Americans in Maine over the past twenty years. This evaluation should begin with a death certificate review to determine whether race was properly coded for deaths of Native Americans in Maine. If these dramatic, positive changes in cardiovascular-related mortality are confirmed, the Bureau of Health should partner with the tribes, the Indian Health Service and others to secure funding for an in-depth evaluation of this population-based prevention success story! Lessons learned from such an evaluation would have tremendous implications.- Devising a mutual strategy to develop and enhance primary and secondary prevention
efforts directed by and toward the Native American population of Maine. Such a strategy should address funding and staffing an integrated, comprehensive prevention program(s) that focuses on each tribe’s particular concern but would probably include such areas as: tobacco and other addictions, physical activity, environmental toxins, nutrition, physical activity, dental, mental and sexual health.
In addition, the Bureau of Health might be helpful to the tribes in working with other state and federal partners to develop strategies to address the complex issues of increasing access to mental health and chemical addiction treatment and devising strategies to provide better major medical—particularly catastrophic --- coverage for un- and under-insured tribal members.
References
Finnegan, L and Ervin, N. E. An epidemiological approach to community assessment. Public Health Nursing, 6(3), 147-51.
Hahn, R. A. and Eberhardt, S. Life expectancy in four U.S. racial/ethnic
populations: 1990. Epidemiology 6,(4), 350-355.
Maine Department of Human Services, Bureau of Health. Maine health 1999:
A health planning resource. Augusta, Maine.
Sorlie, P. D., Rogot, E., Johnson, N. Validity of demographic characteristics on the death certificate. Epidemiology 3,(3), 181-184.